Harness the excitement and eliminate the confusion in cell and gene therapies
The introduction of Chimeric Antigen Receptor T-cell therapy (CAR-T) in the early 2000s was a pivotal tipping point in the evolution of cell and gene therapies. Since then, advancements happen at a feverish pace and market growth is exponential. In 2012, there were 12 CAR-T clinical trials. By 2019, the number surged to 514. And between 2017 and 2020, three CAR-T products reached commercialization, with the number estimated to reach double digits by 2024.
Two therapies that work differently
Both cell and gene therapies treat, prevent and cure genetic and acquired diseases. Cell therapies replace or repair damaged tissues or cells with transplanted human cells. The applications are expansive, as there are hundreds of cells that make up the human body.
Gene therapies, by contrast, replace genes to help the body fight or treat disease, turn off genes that cause problems or replace genes that cause problems with ones that work correctly. Once a new gene is created, a vector is used to deliver new genes directly into cells--either inside or outside the body.
Currently, most of the therapies use products derived from blood samples. But with growing momentum to develop treatments for solid tumors and other tissues, more products with different requirements are likely to emerge.
A simple but challenging supply chain
The raw materials used to develop potentially life-saving cell and gene therapies are most often a patient’s own cells. A trained medical professional collects the cells, ships them to another facility to create the therapy and the therapy is shipped back to the patient’s medical facility for infusion.
However, medical facilities vary in infrastructure, available equipment and technologies. This poses a challenge when temperature-sensitive cells require temperature control and specialized packaging to transport them safely to a biotech company. Facilities may not have equipment to refrigerate or freeze cells, space to store bulky temperature-controlled packaging or appropriate freezers to condition packaging components. Staff familiarity with and training on temperature-controlled packaging could also introduce risk in the form of temperature excursions.
An equally simple solution
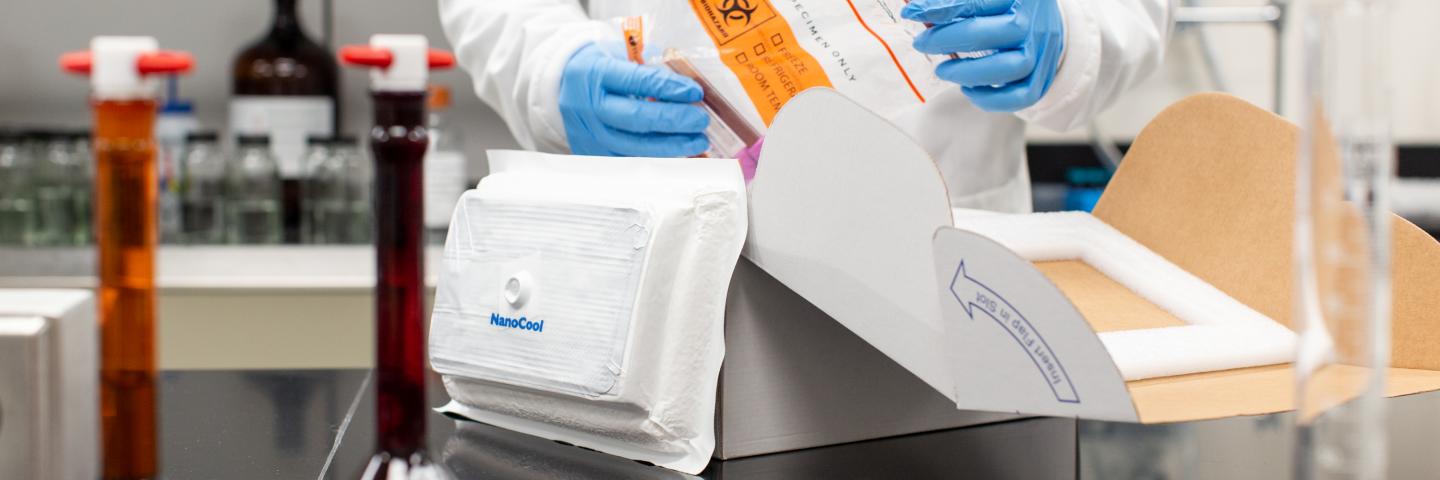
Peli BioThermal single-use and reusable NanoCool™ push button activation refrigerated shippers require no conditioning, and they weigh significantly less than shippers that use traditional coolants like ice. Just one touch of a button activates the cooling process for refrigerated samples, bringing a room temperature product slowly to 2-8 degrees Celsius.
These systems use evaporative, reactive cooling technology that responds and adjusts to varying ambient temperatures. This ensures the payload is protected from external temperature fluctuations throughout the duration of the shipping process.
Therapies shipped back to a patient’s medical facility are most often shipped frozen using vaporized liquid nitrogen (LN2). This requires special training and proves costly because of the specialized training needed to use LN2 shippers. NanoCool DeepFreeze™ dry ice shippers replace LN2 shippers and reduce space and transportation costs.

From clinical trials to commercialization
When moving from one-to-one therapies to commercialized, mass-produced therapies, adaptability and standardization of temperature requirements, packaging and tracking become increasingly important. Biotech companies, cold chain companies and other stakeholders will need to work together to standardize product requirements, maximize efficiencies and optimize benefits for patients who depend on cell and gene therapies.
